How To Build Strong Bones Naturally
“The osteoporosis problem in America is related to several factors, including our overconsumption of salt, soft drinks, caffeine, refined carbohydrates, excess vitamin A (retinal) from animal foods, and alcohol, as well as smoking. All leach calcium and other important nutrients out of the bone,” states Kimberly Gomer, Director of Nutrition and educator at the Pritikin Longevity Center.

Before getting into the subject of strengthening bones naturally, let’s back up a bit and discuss bones themselves – how we build bone, and how we lose it.
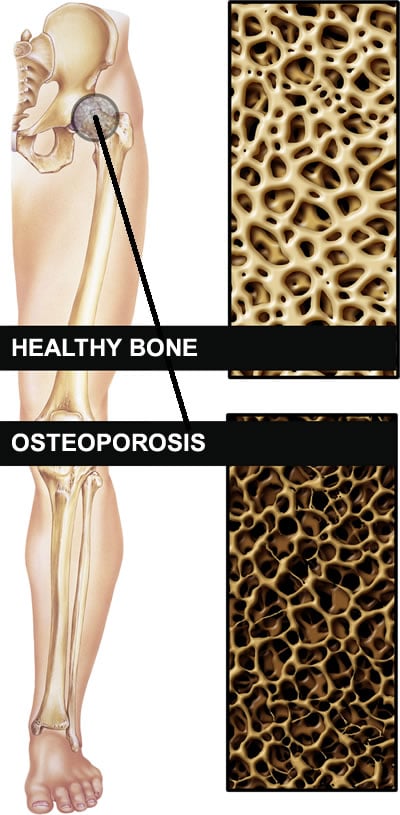
Our bones are in a constant cycle of renewal. Old bone is broken down. And new bone is built.
Building Bone
When we’re young, our body builds new bone faster than it breaks down old. Most of us reach peak bone mass by age 25.
Losing Bone
Usually around age 30, the reverse begins happening. We start losing bone faster than it’s made.
By menopause (and for men about age 60), small holes like broken spider webs begin to appear in the calcium crystals that hold bone together. These holes can grow and grow until bones begin to crumble. A simple fall shatters a hip. “Even a cough, as harmless as it seems, can break a rib,” notes Danine Fruge, MD, ABFP, Medical Director and educator at the Pritikin Longevity Center.
Sometimes, spinal fractures can occur even if you haven’t fallen. The bones that form the spine simply weaken to the point where they collapse, causing back pain, lost height, and a hunchback.
What Is Osteopenia? Osteoporosis?
Put simply, osteopenia is reduced bone mass, and osteoporosis is very reduced bone mass. With osteoporosis, fracture risk is high.
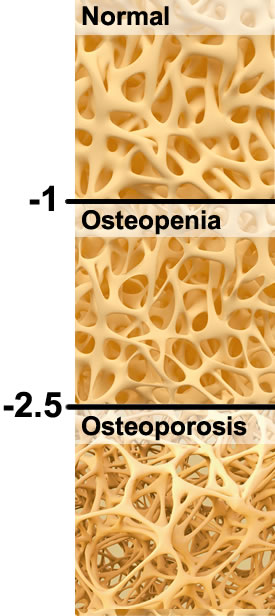
You can determine if you have osteopenia or osteoporosis with a bone mineral density test. You’ll get a T-score. (See pictorial graph.)
How To Prevent Bone Loss and Fractures
“We’ll begin with the sobering news,” acknowledges Dr. Fruge. “We have no control over some risk factors for osteoporosis.” They include:
- Being female. Women are much more likely to develop osteoporosis than men (but men are not immune).
- Getting older
- Being of white or Asian descent
- Having a family history of osteoporosis
- Having a small body frame. People with small body frames tend to be at higher risk because they have less bone mass to begin with.
“But other key risk factors are lifestyle related, which means there’s much that’s in our power to help keep our bones strong,” assures Dr. Fruge.
Two important lifestyle factors are physical activity and diet.
How To Build Strong Bones Naturally
Physical Activity, Especially Resistance Training
Studies on weight-bearing exercises, particularly resistance training such as weightlifting, have shown significant gains in bone mass in older men and women.
But even if bone loss can’t be stopped, “keep exercising,” encourages Dr. Fruge. “Exercise builds muscles. Having strong muscles means you’re less likely to fall.”
More than 90% of hip fractures are the immediate consequence of a fall. “Fall prevention is a priority for patients with osteoporosis,” emphasized recent guidelines1 on managing osteoporosis from the American Academy of Family Physicians.
Other important tips for preventing falls and consequent fractures include:
- Take classes, such as yoga and functional fitness, that improve balance and agility
- Get rid of throw rugs in the house
- Use non-slip bathmats
- Add handrails and lights in all staircases
- Install nightlights, especially from bedroom to bathroom
- Incorporate small (but highly beneficial) balance and strength exercises into daily living, such as standing on tiptoe while waiting in line at the market
How To Build Strong Bones Naturally
Dietary Factors
“The osteoporosis problem in America is related to several factors, including our overconsumption of salt, soft drinks, caffeine, refined carbohydrates, excess vitamin A (retinal) from animal foods, and alcohol, as well as smoking. All leach calcium and other important nutrients out of the bone,” states Kimberly Gomer, MS, RD, LDN, Director of Nutrition and educator at the Pritikin Longevity Center.
Conversely, the Pritikin Eating Plan, which is taught at the health resort, is a rich source of virtually all the nutrients, including calcium, that help keep bones strong. Dairy is important but so are fish, beans, and produce. In fact, collard greens have as much calcium per cup as milk.
Bone-Building Stars
| Green Leafy Vegetables (cooked, per cup) | Calcium (mg) |
|---|---|
| Collard greens | 300 |
| Turnip greens | 229 |
| Bok choy | 200 |
| Kale | 179 |
| Mustard greens | 150 |
| Broccoli | 150 |
| Artichoke (1 large) | 102 |
| Fish | |
|---|---|
| Sardines (with bones, 3½-oz can) | 300 |
| Oysters (raw, 1 cup) | 226 |
| Salmon (canned with bones, 3 oz) | 199 |
| Beans and Legumes | |
|---|---|
| Tempeh (4 oz) | 172 |
| Garbanzo beans (1 cup, cooked) | 150 |
| Tofu – firm (4 oz) | 150 |
| Black beans (1 cup, cooked) | 135 |
| Pinto beans (1 cup, cooked) | 128 |
| Dairy | |
|---|---|
| Ricotta cheese, nonfat (1/2 cup) | 337 |
| Milk (nonfat, 1 cup) | 300 |
| Yogurt (nonfat, 1 cup) | 300 |
| Mineral Waters | |
|---|---|
| San Pellegrino (1 liter) | 200 |
| Perrier (1 liter) | 140 |
| Other Sources | |
|---|---|
| Sesame seeds (1/4 cup) | 352 |
| Soymilk (calcium fortified, 1 cup) | 300 |
| Almonds (1/4 cup) | 150 |
| Corn tortillas (two) | 120 |
How Is Your Renal Acid Load?
Fruits and vegetables are also vital for strong bones because they have a beneficial effect on renal acid load.
To preserve bone, we don’t want a renal acid load that’s high. Unfortunately, certain foods in a typical American diet lead to high renal acid loads. One major contributor is grains. (Interestingly, acidic foods like citrus fruit do not create acid in the body.) The high renal acid load produced by grain-rich diets is generally not handled well by older people because of declining kidney function. To neutralize the excess acid in the bloodstream, the body breaks down muscle and bone, which leads to osteoporosis.
Fruits and vegetables, by contrast, add alkali to the body, which helps to neutralize the acid.
“Bottom line, when a diet is low in fruits and vegetables and high in grains, there is a net acid-producing effect, which is detrimental to bones,” sums up Kimberly Gomer, MS, RD, Director of Nutrition at Pritikin.
“So make sure you’re eating plenty of fruits and vegetables, as we recommend with the Pritikin Eating Plan.”
Calcium Supplements | Do You Need Them?
“If you are following a plant-based, whole foods diet like Pritikin and exercising regularly, chances are you do not need calcium supplementation,” states Gomer.
With Pritikin’s rich amounts of bone-building nutrients, including calcium, you’re probably taking in about 800 to 1,000 mg of calcium daily.
True, this amount is slightly less than the current RDAs of 1,000 to 1,200 mg of calcium for older American adults, “but our country’s RDAs are high, and they’re high because our typical U.S. diet is high in calcium leachers like salt, meat, and refined grains. When you’re eating the typical U.S. diet, you probably do have significant calcium losses. But when you’re eating a healthy Pritikin diet and exercising regularly, you’re losing less calcium, which means you likely need less,” explains Gomer.
Moreover, research has found that calcium supplementation has, at best, marginal success in preventing fractures.2
And calcium supplementation may do more harm than good. Some large studies have linked calcium supplements to an increased risk of serious health problems, including kidney stones, acute gastrointestinal events, heart attacks, and strokes. In a NIH-AARP study,3 for example, 388,229 men and women initially aged 50 to 71 were followed for an average of 12 years. Taking supplemental calcium raised the risk of cardiovascular-related death by 20% among men.
However, a large meta-analysis4 of 4 randomized trials and 27 observational studies found that calcium intake within RDA intake levels “is not associated with cardiovascular disease risk in generally healthy adults.”
Food Sources, Not Supplements
Certainly, more research is needed. In the meantime, “the safest and most effective source of calcium and other nutrients for strong bones is food sources, not supplements,” states Dr. Fruge. “A food plan like Pritikin is likely best for bone health, and certainly, it’s best for overall health, particularly cardiovascular health.
“If you, in consultation with your doctor, choose to take calcium supplements, our recommended form is calcium citrate because it’s absorbed even if you don’t have a lot of acid in your stomach, a deficiency that is common as people age.”
Calcium carbonate, the type of calcium found in popular antacids, is not readily absorbed in those with acid deficiency. If you take an antacid, take it with food. Calcium citrate works with or without food.
Vitamin D Supplements | Do You Need Them?
Vitamin D is vital for strong bones. It helps absorb calcium into the bone. Fortified milk and soymilk are good sources, as is the sun.
It’s a good idea to have your vitamin D level assessed via blood testing. Many Americans, even those in sunny climates, have been found to be vitamin D deficient.
Factors that may lower blood levels of vitamin D include obesity, living in northern latitudes (above Atlanta on the east coast and Los Angeles in the west) religious covering of the skin, and natural pigment level of skin.
What are optimal blood levels of vitamin D? At this point in time, scientific research has not given us an exact number, which means that health organizations often have varying recommendations. But large randomized controlled trials, including the VITAL Study, are underway. Our hope is that in the near future these trials will provide us with more precise answers.
Recommended Ranges
From the data currently available, the physicians, dietitians, scientists, and other faculty that make up the Pritikin Scientific Advisory Board recommend blood levels of vitamin D in the range of 25 to 50 ng/mL. This range appears to offer bone-preserving benefits but with no negative side effects.
Do discuss your vitamin D needs with your physician because, based on your medical history, your goals may be different. If blood testing shows you are deficient in vitamin D, your physician can prescribe appropriate supplementation to correct the deficiency.
Keep in mind that increases in blood levels of vitamin D may take several months, maybe a year. To monitor your progress, have your vitamin D level tested regularly.
Other Factors Related To Bone Loss
- Lowered sex hormone levels
The decrease of estrogen levels at menopause is a strong risk factor for osteoporosis. - Increased thyroid hormone levels
Increased levels may occur if your thyroid is overactive or if you are taking too much thyroid hormone medication to treat an underactive thyroid. - Gastrointestinal surgery
Reductions in stomach size, or bypasses or removal of part of the intestine, can reduce the ability to absorb nutrients, including calcium. - Steroids and other medications
Long-term use of corticosteroid medications, such as prednisone and cortisone, may interfere with bone-rebuilding. Osteoporosis has also been linked with medications for gastric reflux, seizures, cancer, and transplant rejection.
How To Build Strong Bones Naturally | Key Takeaways
Important lifestyle-based measures for preventing osteoporosis include:
- Daily exercise for muscle toning and strength, and
- A well-balanced, nutrient-rich diet like the Pritikin Eating Plan
“Never underestimate the power of a healthy lifestyle like Pritikin to keep both heart and bones strong,” sums up Dr. Fruge.
Osteoporosis
If you are diagnosed with osteoporosis, pharmacological therapies involve two basic types: antiresorptive medications, which slow the breakdown of bone; and anabolic medications, which help to make new bone.
“And certainly, routine follow-ups with bone mineral density testing should be performed to monitor the health of your bones,” adds Dr. Fruge.
“We have guests who return annually for health vacations at Pritikin. While here, many have their bones checked with bone mineral density testing, and they’re often very pleased with the results.”